Typically, an anion gap greater than 20 mmol/L may be considered as high anion gaps greater than 18 mmol/L should be further investigated. Metabolic acidosis can have a normal or high anion gap, where the anion gap refers to difference between the number of cations (i.e., sodium and potassium ) and the number of anions (i.e., chloride and HCO 3 –). Metabolic acidosis is defined as an excess in non-volatile acid load that results in a primary decrease in plasma bicarbonate (HCO 3 –) associated with a low plasma pH. Metabolism of sulfur-containing amino acids (i.e., methionine and cysteine) yields sulfuric acid, while dietary phosphate yields phosphoric acid. The amino acids lysine and arginine are metabolized to generate acids, while metabolism of glutamate and aspartate and organic anions, such as acetate and citrate, yield alkali. In healthy individuals ingesting a typical Western diet, metabolism produces acid or alkali components, with a daily net acid production of approximately 1 mmol/kg of body weight per day.

The maintenance of acid–base homeostasis is a major function of the body, accomplished by intracellular and extracellular buffering mechanisms, exhalation of carbon dioxide (CO 2) through the respiratory system, and acid excretion by the kidneys.
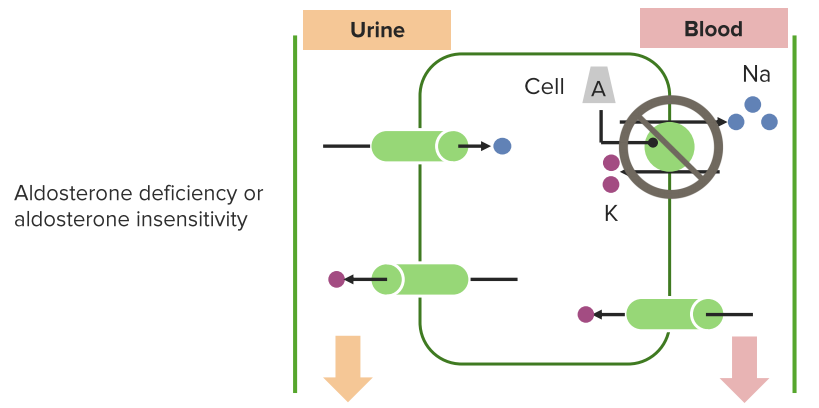
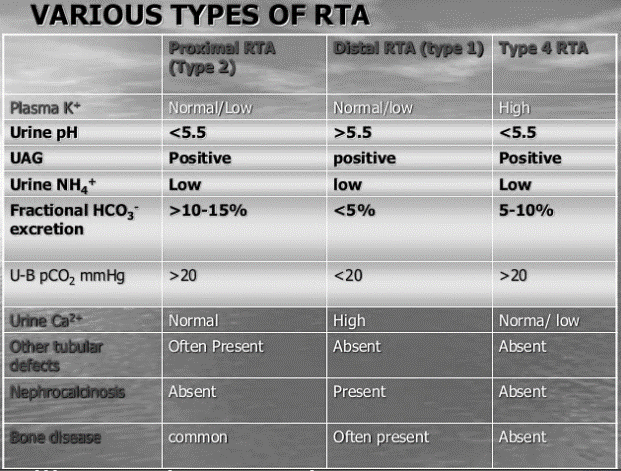
Treatment options include alkali therapy in patients with distal or proximal RTA and lowering of serum potassium concentrations through dietary modification and potential new pharmacotherapies in patients with hyperkalemic RTA including newer potassium binders. The diagnosis of distal versus proximal RTA involves assessment of urinary acid and bicarbonate secretion, while in hyperkalemic RTA, selective aldosterone deficiency or resistance to its effects is confirmed after exclusion of other causes of hyperkalemia. Accurate diagnosis of RTA plays an important role in optimal patient management. Type 3 RTA is a rare form of the disease with features of both distal and proximal RTA. The three major forms of RTA are distal RTA (type 1 characterized by impaired acid excretion), proximal RTA (type 2 caused by defects in reabsorption of filtered bicarbonate), and hyperkalemic RTA (type 4 caused by abnormal excretion of acid and potassium in the collecting duct). Using illustrative clinical cases, this review describes the main types of RTA observed in clinical practice and provides an overview of their diagnosis and treatment. Renal tubular acidosis (RTA) occurs when the kidneys are unable to maintain normal acid−base homeostasis because of tubular defects in acid excretion or bicarbonate ion reabsorption.
